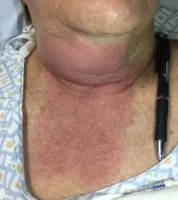
 Case: A 78 year-old female with a past medical history of asthma and hypothyroidism presents with a three day history of sore throat and a two day history of a “lump” along the right side of her neck. The “lump” has now progressed to involve both sides of her anterior neck and is accompanied with erythema, tenderness to palpation, and swelling. In addition, the patient has developed a hoarse voice and odynophagia. The patient’s primary care physician referred her to an ENT specialist, who then referred the patient to the ED for urgent imaging due to the concern for a deep space neck infection. Triage vitals are remarkable for a heart rate of 118 beats per minute. She is otherwise normotensive and afebrile. On physical exam, slight crepitation in noted on the floor of the patient’s mouth. Of note, the patient also informs you of her penicillin allergy. Which of the following is the biggest risk factor for this particular disease process?
Case: A 78 year-old female with a past medical history of asthma and hypothyroidism presents with a three day history of sore throat and a two day history of a “lump” along the right side of her neck. The “lump” has now progressed to involve both sides of her anterior neck and is accompanied with erythema, tenderness to palpation, and swelling. In addition, the patient has developed a hoarse voice and odynophagia. The patient’s primary care physician referred her to an ENT specialist, who then referred the patient to the ED for urgent imaging due to the concern for a deep space neck infection. Triage vitals are remarkable for a heart rate of 118 beats per minute. She is otherwise normotensive and afebrile. On physical exam, slight crepitation in noted on the floor of the patient’s mouth. Of note, the patient also informs you of her penicillin allergy. Which of the following is the biggest risk factor for this particular disease process?
Poll Results
[plot id=”1″]
[su_spoiler title=”Answer” style=”fancy” icon=”caret”]
Dental infections are the biggest risk factor for Ludwig’s Angina
Explanation
Ludwig’s Angina is an infection of the bilateral submandibular space, usually beginning on the floor of the mouth and spreading aggressively to the submandibular space, often accompanied by cellulitis. Without treatment, this process has a mortality rate of up to 50% from asphyxia— now, with the advent of antibiotics and early recognition, the mortality of this disease is less than 10%.1
Typical symptoms include fever, chills, mouth pain, neck stiffness, drooling, changes in voice, and dysphagia.1 On exam, patients tend to have symmetric induration, occasional palpable crepitation in the submandibular region, and the floor of the mouth can be elevated, tender to palpation and erythematous.1,2
Accompanying abscess formation is rare, so there is usually nothing to drain.3 Over 65% of Ludwig’s angina cases have a dental source of infection, predominantly involving the 2rd or 3rd molars.4 Other potential sources of infection include contiguous spread from a peritonsillar abscess or from parotitis.4
The infection usually is polymicrobial in nature with anaerobic involvement. Accordingly, suggested initial antibiotic regimens include (ampicillin-sulbactam 3 g every 6 hours, or clindamycin 600 mg IV every 6-8 hours, or penicillin G 2-4 mg every 4 to 6 hours) plus metronidazole 500 mg IV every 6-8 hours. Carbapenems should be considered in immunocompromised individuals due to the high prevalence of and susceptibility to gram-negative anaerobes in this population.
To confirm the nature of the deep space neck infection, experts recommend CT as the initial imaging modality of choice unless there is impending airway compromise.
The biggest concern for ED providers should focus on airway protection and swift involvement of ENT specialists if needed. If the airway is a concern, the suggested route of control is via nasal fiberoptic intubation or surgical tracheostomy.2
Case Conclusion
An emergent CT scan and ENT consultation were obtained in the ED. The patient did not require any airway intervention. The CT scan confirmed the presence of Ludwig’s angina and the patient was started on an IV antibiotic regimen and IV dexamethasone in the ED. Given the patient’s penicillin allergy, the patient was started on vancomycin, aztreonam, and metronidazole. The patient’s clinical symptoms improved and the patient’s blood cultures grew Streptococcous anginosus. The patient was discharged home after a week-long stay in the hospital and continued to improve when seen by the ENT specialist as an outpatient.
Interestingly, the patient did not have a dental source of her infection and the nidus for the infection continues to remain unclear.
[/su_spoiler]
Master Clinician Bedside Pearls
Edward Klofas, MD
Clinical Associate Professor of Emergency Medicine
Stanford University
Author information
The post Diagnose on Sight: Case of a red, swollen neck appeared first on ALiEM.

