 Background Information:
Background Information:
Double external defibrillation (DED) is an intervention often used to treat refractory ventricular fibrillation (RVF). This procedure involves applying another set of pads attached to a second defibrillator to a patient and shocking them in hopes of terminating the rhythm. At REBEL EM, we’ve done an extensive write up that details some of the different types of DED and the electrophysiology behind it. That write up was for the DOSE-VF pilot trial done in March 2020 and can be found here. Now that same group has published the results of their full randomized control trial. The authors sought to answer whether double defibrillation and/or vector change defibrillation lead to a greater number of RVF patients surviving to hospital discharge when compared to standard defibrillation therapy.
REBEL Cast Ep113 – Defibrillation Strategies for Refractory Ventricular Fibrillation
Paper: Cheskes S, et al. Defibrillation Strategies for Refractory Ventricular Fibrillation. N Engl J Med. 2022 Nov 6 PMID: 36342151
Clinical Question:
- How does double defibrillation and vector change defibrillation compare to standard therapy in OHCA patients with refractory ventricular fibrillation?
What They Did:
- Three-arm pilot randomized control trial with a randomized cluster crossing period, conducted across six paramedic services in Ontario, Canada
- The study occurred from March 2018 to May 2022 with a pause from April 2020 to September 2020 to address concerns about paramedics performing aerosolizing procedures during the COVID-19 pandemic
- One of the three following defibrillation strategies was assigned through computer-generated randomization to one of the six regional paramedic services and performed after three standard defibrillation attempts by either responding paramedics or participating fire services:
- Strategy 1: Continued standard defibrillation therapy with pads in the anterior-lateral configuration
- Strategy 2: Vector change (VC) defibrillation with pads transferred from the standard anterior-lateral to the anterior-posterior position
- Strategy 3: DSED with pads in the anterior-posterior position and an intentional delay to ensure rapid sequence delivery vs simultaneous defibrillation
- Prehospital care was provided by “advanced care” paramedics who perform full ACLS and are assisted by “primary care” paramedics who perform basic life support skills with the addition of a small number of medications and manual defibrillation
- Cluster crossing over meant that each of the paramedic services in the six regions was randomized to one of the three treatment approaches and then crossed over to an alternate defibrillation strategy every 6 months.
- To avoid possible defibrillator damage, double sequential and not simultaneous defibrillation was performed. Meaning an intentional short delay of <1 second between the shocks was implemented (more on this in discussion section)
- The trial was stopped early due to longer prehospital response times secondary to staffing shortages interfering with the timely delivery of the assigned defibrillation strategy
Inclusion Criteria:
- Adult patients over the age of 18 years old
- Non-traumatic OHCA of presumed cardiac etiology
- Remaining in refractory VF or pulseless ventricular tachycardia after three standard defibrillation shocks
Exclusion Criteria:
- Traumatic cardiac arrest
- Pre-existing do not resuscitate orders
- Cardiac arrest secondary to drowning, hypothermia, hanging or suspected drug overdose
- Patients being treated by non-participating fire or EMS agencies who did not get three shocks
Outcomes:
Primary
- Survival to hospital discharge
Secondary
- Termination of ventricular fibrillation on subsequent rhythm analysis after defibrillation and 2 minutes of CPR
- Return of spontaneous circulation (ROSC), defined as any change in rhythm to an organized rhythm with a corresponding palpable pulse and blood pressure
- Good neurologic outcome, defined as a modified Rankin score of < 2
Results:
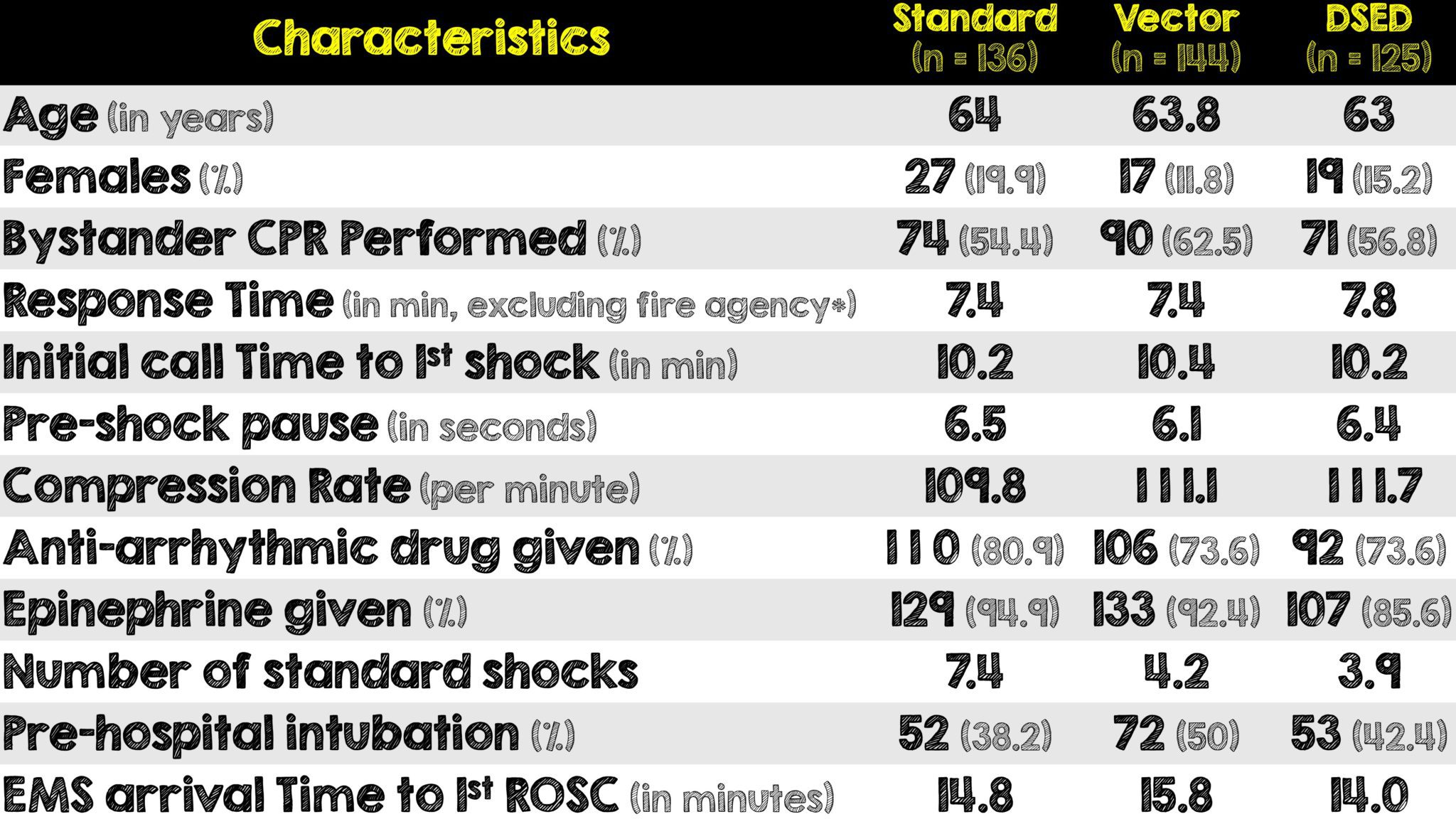
- 450 patients were enrolled and a total of 405 underwent randomization
- Five patients were found to be in pulseless ventricular tachycardia, 2 in the standard arm, 2 in the VC arm and 1 in the DSED arm
Critical Results:

Strengths:
- First randomized control trial to compare the use of a second external defibrillator and pad placement change to standard therapy
- Patient oriented primary and secondary outcome looking at survival to discharge and neurologic status
- Cluster crossover approach was done to maximize efficiency by comparing two new treatments to usual care
- Extremely well-trained paramedics with a high level of oversight who got extra training in CPR and the protocol of the study/performing DED
- Utilized multiple paramedic services in both urban and rural settings to reflect real practice
- Incredibly fast response times well above the EMS standard in the United States
Limitations:
- Trial stopped early and thus potentially overestimating the benefit
- No fixed follow-up time was set and mRS was abstracted from discharge summaries with no other follow-up (in-person or virtual) reported
- Unblinded trial opens up providers in the study to Hawthorne Effect bias (ie. trying harder and longer knowing they are enrolled in this study)
- Use of two different models of defibrillators may negatively impact the internal validity of this pilot study
- Certain baseline characteristics were not balanced, such as: prehospital intubation and Epinephrine administration.
- All energy delivered by the ZOLL defibrillators in the first three shocks were lower than the first shock delivered by the LifePak 15 which may serve as a confounding variable as a higher amount of energy delivered earlier may skew results
- External validity limited to regions with this extensive pre-hospital training with very high physician involvement
- The EMS system in Ontario, Canada consists of two paramedics able to perform manual defibrillation. Within the United States, due to paramedic shortages, this dual-medic setup does not exist in many EMS systems.
- Race, ethnicity, outpatient medications and other data was not collected raising the concern of other confounding variable that may have impacted patient outcomes
- Paramedics failed to adhere to study protocol
Discussion:
- DISCLOSURE: I have previously published work related to double defibrillation and know the principal investigator on a personal level. The following commentary is my best attempt at an unbiased approach.
- The prehospital providers in this study had an extensive amount of training. In fact, 4000 paramedics in total were not only trained in the study protocol but also given a rigorous evaluation of their ability to perform CPR. This in addition to an already high amount of oversight is not something you will find in most EMS systems. Thus limiting the external validity of this paper’s findings.
- Paramedics failed to adhere to the study protocol, causing some patients who were supposed to receive VC defibrillation or DSED to receive standard defibrillation. Having worked as a paramedic in the past and given the nature of prehospital medicine, this understandably can happen. I bring this up because it must be considered when interpreting the overall results and benefits of the study.
- On the topic of EMS and similar to the pilot study, there was an incredibly high amount of bystander CPR performed. This was in addition to a phenomenally fast EMS response time. Unfortunately, neither of these occur at such a high frequency here in the United States thus even further limiting the external validity of this paper.
- This trial was performed in Ontario, Canada which, as part of a socialized healthcare system, has much easier access to in-hospital records across the entire province. While many healthcare systems across the world operate in a similar fashion, the United States does not.
- While the methodology of this study remains very good for an unblinded trial, I have some concerns regarding the consistency of data reporting. They stated that DSED was performed on pulseless ventricular tachycardia (pVT) however it was not reported exactly how many patients were in pVT and I had to contact the PI to obtain this information
- Although DED and VC performed better than standard therapy, the confidence intervals overlap when compared with VC. It’s difficult to definitively say which of the two is statistically better, however there is a trend pointing toward DED. The fragility index of these findings found to be 1 for VC and 9 for DED
- Obtaining a second defibrillator in the emergency department or intensive care unit can be very easy to do. However, when practically applying the results of this study in the prehospital setting, EMS agencies will need to strongly consider how this will operationally and impact their workflow and the number of other ambulances or supervisors available with a second defibrillator. In most cases, prehospital cardiac arrests often necessitate a second ambulance crew simply to assist with compressions, patient transfer or medication administration anyway.
- The above resource limitation applies in the opposite setting and requires a clinical judgement call to be made. If you work in a tertiary academic center with a catheterization lab and/or ECMO immediately available, the application of a second defibrillator may not be immediately needed. Depending on the scenario, it should likely be reserved as a temporizing measuring if there are delays in mobilizing these interventions.
- As mentioned above we’ve talked before on REBEL EM about the difference between Double Simultaneous vs Double Sequential defibrillation. It’s impossible without the use of an oscilloscope to know which we are performing. This study intentionally performed double sequential defibrillation to avoid defibrillator damage and in their pilot study referenced a flawed case report as to why simultaneous was not performed. I believe this trial was a missed opportunity to perform simultaneous defibrillation as a fourth arm to better investigate which of the two methods of performing this have more efficacy as we’ll now need to wait for additional trials to be performed to evaluate this.
- Speaking of defibrillator damage, not a single defibrillator was damaged during this trial. .
- If double defibrillation is going to be implemented in your institution or EMS agency it’s imperative that you know the following to avoid damaging your devices:
- Use the SAME model of defibrillator
- Pads need to be close as possible but NOT touching to avoid capacitor overload
- NEVER hit the synchronization button (this shouldn’t be done anyway if using it for RVF but it needs to be said)
- This study is certainly a step in the right direction and what it may do is start the discussion with many of the guideline writing organizations to include more information about double defibrillation in their algorithms. I am hopeful this trial encourages future research on the subject matter so we can answer additional questions it has left us (ie. sequential vs simultaneous, earlier vs later double defibrillation, larger pads or higher energy from the onset, etc)
- Interpretation of this study needs to occur with caution as there are many system-wide characteristics in its design that cannot be applied to most institutions and EMS agencies. The early termination is also a concern and may have overestimated the benefits of this intervention.
- With everything just mentioned considered, DED, in addition to other resuscitative therapies, should still be used for patients in RVF. Following the results of this trial, thorough discussions should be had regarding its feasible and practical implementation across institutions and EMS agencies.
Author’s Conclusions:
- Among patients with refractory ventricular fibrillation, survival to hospital discharge occurred more frequently among those who received DSED or VC defibrillation than among those who received standard defibrillation
Our Conclusion:
- The findings of this unblinded randomized control trial need to be cautiously interpreted due to many methodological characteristics that limit its external validity. This study should certainly prompt discussions about the operational feasibility when it comes to implementing DED across institutions and EMS agencies. Although additional research is needed before considering double defibrillation the standard of care, it should still be considered in patients with RVF. If a second defibrillator is unavailable, consideration should be given to changing pad placement from anterolateral to anteroposterior when performing defibrillation with a single device.
Clinical Bottom Line:
- Double sequential defibrillation and vector change defibrillation are both feasible treatments for refractory ventricular fibrillation with the later being more practical and cost effective in the prehospital setting. . However, until additional evidence presents itself, the use of double defibrillation on a case-by-case basis should be considered based on operational feasibility such as institution/agency policies, and availability of resources.
REFERENCES:
- Cheskes S, et al. Defibrillation Strategies for Refractory Ventricular Fibrillation. N Engl J Med. 2022 Nov 6 PMID: 36342151
- Cheskes S, et al. Double sequential external defibrillation for refractory ventricular fibrillation: The DOSE VF pilot randomized controlled trial. Resuscitation 2020; PMID: 32084567
- REBEL EM: Dual Sequential Defibrillation (DSD)
- REBEL EM: Beyond ACLS: Dual Simultaneous External Defibrillation
- EmCrit: Dual External Defibrillation: Close but Not Touching
- First10EM: Dose VF: A double sequential defibrillation game changer?
- The Bottom Line: Defibrillation Strategies for Refractory Ventricular Fibrillation
- St. Emlyn’s Blog: Alternate Defibrillation Strategies in Refractory VF
Post Peer Reviewed By: Salim Rezaie, MD (Twitter: @srrezaie)
The post REBEL Cast Ep113: Defibrillation Strategies for Refractory Ventricular Fibrillation appeared first on REBEL EM - Emergency Medicine Blog.
