
 Background/Introduction: Emergency department visits related to cannabis use appear to be increasing nationally secondary to continued trends of legalization, decriminalization, or less restrictive medical cannabis use laws in many states. The number of individuals with daily cannabis use in the United States increased from 5.1 million in 2005 to 8.1 million in 2013 (Bollom 2018). With an increase in the accessibility and consumption of cannabis, there has also been an increase in the utilization of emergency departments for potential adverse effects of cannabis use, particularly gastrointestinal adverse effects. For example, in Colorado, the emergency department visits for cyclic vomiting nearly doubled after liberalization of medical marijuana (Kim 2015). Studies attempting to look at nationwide sampling have noted that the number of persistent vomiting related hospitalization related to cannabis use had a significantly increased trend, with a 286% increase over a 5-year period (Patel 2019).
Background/Introduction: Emergency department visits related to cannabis use appear to be increasing nationally secondary to continued trends of legalization, decriminalization, or less restrictive medical cannabis use laws in many states. The number of individuals with daily cannabis use in the United States increased from 5.1 million in 2005 to 8.1 million in 2013 (Bollom 2018). With an increase in the accessibility and consumption of cannabis, there has also been an increase in the utilization of emergency departments for potential adverse effects of cannabis use, particularly gastrointestinal adverse effects. For example, in Colorado, the emergency department visits for cyclic vomiting nearly doubled after liberalization of medical marijuana (Kim 2015). Studies attempting to look at nationwide sampling have noted that the number of persistent vomiting related hospitalization related to cannabis use had a significantly increased trend, with a 286% increase over a 5-year period (Patel 2019).
This has led to a renewed interest in the understanding of cannabis hyperemesis syndrome, first well-described in 2004, and recently defined by the Rome IV criteria (Allen 2004). The effective management of cannabis hyperemesis syndrome is still being elucidated as commonly used antiemetics are often ineffective for acute exacerbations. The role of haloperidol as an off-label treatment is being explored but anecdotal evidence suggests it may be an effective adjunct in the treatment of cannabis hyperemesis syndrome.
Paper: Ruberto KH et al. Intravenous Haloperidol Versus Ondansetron for Cannabis Hyperemesis Syndrome (HaVOC): A Randomized, Controlled Trial. Ann Emerg Med. 2020. PMID: 33160719
Clinical Question: Is haloperidol superior to ondansetron in the treatment of abdominal pain and nausea in adult emergency department patients with cannabis hyperemesis syndrome?
What They Did:
- Randomized, triple-blinded crossover trial between 2017 and 2019
- 2 academic EDs in Canada
- Patients randomized to:
- Low Dose Haloperidol: 0.05mg/kg IV
- Higher Dose Haloperidol: 0.1mg/kg IV
- Ondansetron 8mg IV
- All patients received 1L of LR over 30 min
- Nausea and abdominal pain scored on a 10-cm VAS
Outcomes:
-
Primary Outcomes:
- Average combined change in nausea and abdominal pain scores at 120min
-
Secondary Efficacy Outcomes:
- Change in either nausea or abdominal pain scores over time
- Treatment success (Defined as both nausea and abdominal pain VAS of <2cm at ≥120min)
- Time to discharge
- Use of rescue antiemetics prior to discharge
- Length of stay >12hrs
- Unscheduled return ED visits within 7d
-
Secondary Safety Outcomes:
- Adverse effects potentially related to the study drug including acute dystonia and moderate to severe akathisia
Inclusion Criteria:
- Adult patients (> 18 years of age)
- Working diagnosis of hyperemesis caused by cannabis (both criteria necessary)
- ≥3 episodes of emesis in a cyclic pattern separated by > 1 month during the preceding 2 years
- Near daily use of cannabis by inhalation for ≥6 months
- > 2 hours of ongoing, witnessed emesis or retching
Exclusion Criteria:
- Known allergy or intolerance to study drug
- Daily opioid use
- Received an antiemetic, anticholinergic, or antipsychotic agent intravenously in the previous 24 hours (other than up to 100 mg dimenhydrinate)
- Pregnancy
- Unreliable or unwilling to follow up
- Unable or unlikely to return for crossover
Results:
- 30 patients randomized
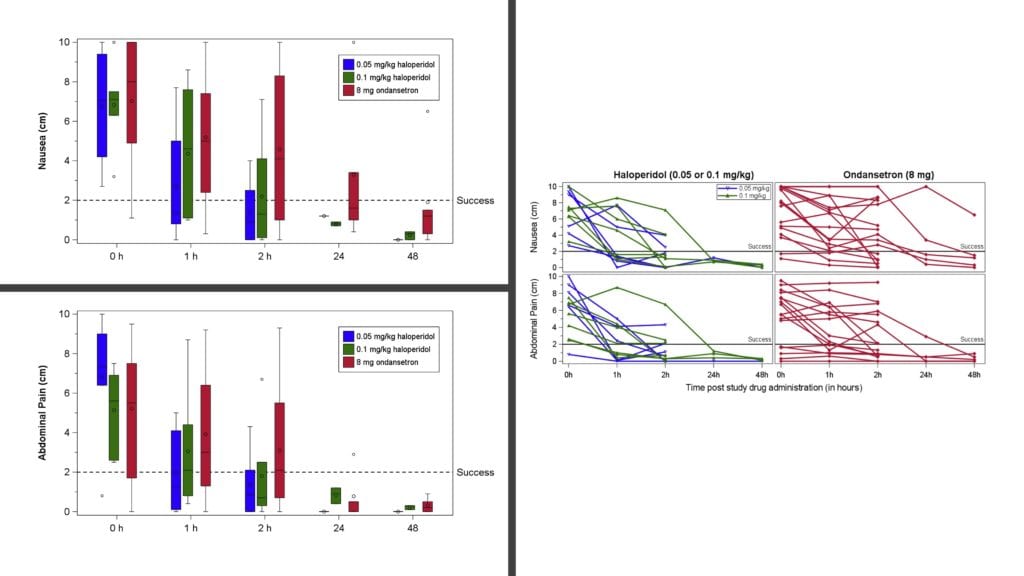
- Efficacy Outcomes:
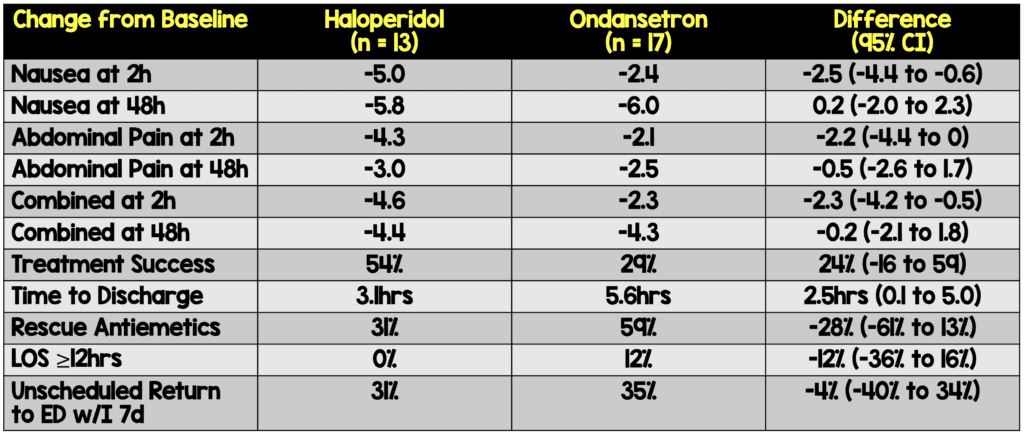
- Either dose of haloperidol was superior to ondansetron for the primary outcome of improvement in nausea and abdominal pain at 120 minutes in patients with cannabis hyperemesis syndrome
- After adjusting for baseline, the mean difference in the primary outcome was 2.3cm (95% CI 0.6 to 4.0cm; p = 0.01) favoring haloperidol
- Haloperidol was also superior to ondansetron for the secondary outcomes of nausea or abdominal pain acutely (at 120 minutes) and was associated with a shorter time to discharge, less use of rescue antiemetics, and a shorter overall emergency department length of stay
- Secondary Safety Outcomes:
- 3 events, all with high dose haloperidol: 1 moderate akathisia reaction and 2 acute dystonic reaction
Strengths:
- Adds information to a question with limited and inconsistent previous research
- Baseline characteristics of the patients were comparable between groups
- No patients lost to follow-up for the primary outcome at 2 hours
- Used 2cm threshold for improvement in both nausea and abdominal. This was prespecified and a threshold widely used to represent a meaningful improvement in either symptom
Limitations:
- Largest limitation was that the trial did not achieve prespecified enrollment target with overall small sample size causing wide confidence intervals in all outcomes
- Low crossover rate between different study drugs and dosing regimens leading to unpaired analysis
- Inadequate 24-hour and 48-hour follow-up data. Only 9 out of 30 patients included in these results
- Narrow inclusion and exclusion criteria
- Findings may not be generalizable to other settings or consistent over time due to high heterogeneity of cannabis and its constituents
- Convenience sample of patients as 201 out of 313 patients were missed which creates an inability to generalize the results and potentially biasing the results
Discussion:
- Blinded, unplanned interim analysis of the trial led to a recommendation to halt the trial due to a strong effect on the primary outcome in favor of one drug treatment
- The average improvement in both nausea and abdominal pain exceeded the prespecified minimal clinically significant difference of 2 cm
- This trial shows that the standard 4mg of ondansetron should no longer be used as a first-line agent to abort emesis in cannabis hyperemesis syndrome, as the 8mg dose did not fare well
- This is an important study that is attempting to clarify the role of a potentially promising medication for the treatment of cannabis hyperemesis syndrome. This will hopefully serve as a jumping off point for future randomized controlled trials and further research into identifying the optimal role of haloperidol and other medications in the treatment of cannabis hyperemesis syndrome.
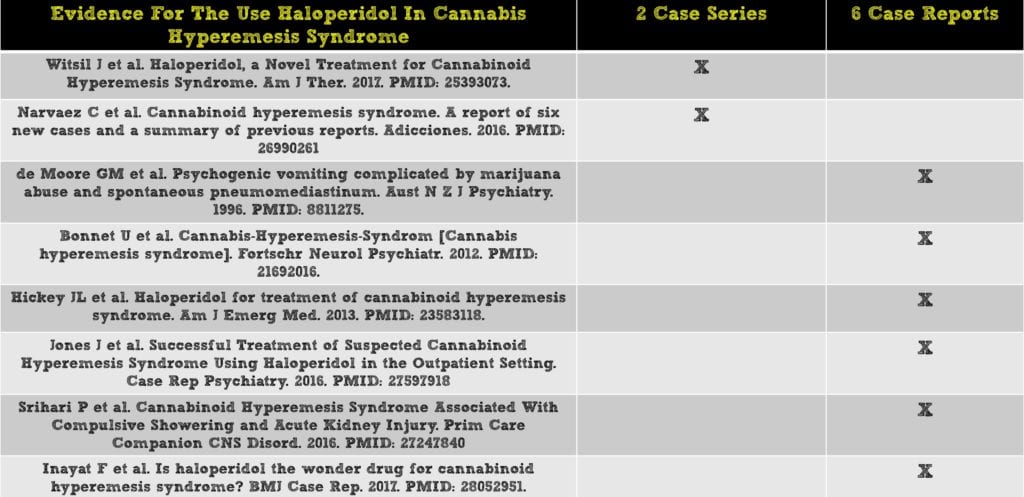
- To date, there have been no randomized controlled trials looking at haloperidol for the effective treatment of cannabis hyperemesis syndrome. There have been multiple case series and case reports that have looked at haloperidol:
Author Conclusion: “In this clinical trial, haloperidol was superior to ondansetron for the acute treatment of cannabis-associated hyperemesis. The efficacy of haloperidol over ondansetron provides insight into the pathophysiology of this now common diagnosis in many EDs.”
Clinical Take Home Point: In this small randomized controlled trial of patients with cannabis hyperemesis syndrome, the use of haloperidol was associated with improvement in the rates of acute (less than 120 minutes) nausea and abdominal pain, shorter emergency departments length of stay, shorter time to discharge, and less use of rescue medications over the commonly used antiemetic ondansetron. The findings need to be interpreted in the context of inadequate sample size, narrow inclusion and exclusion criteria, as well as unpaired analysis due to low crossover rates.
The bottom line is that only cannabis cessation at this time appears to be the most effective treatment modality but supportive care with intravenous fluids, topical capsaicin cream, avoidance of narcotic medications, and the use of dopamine antagonists such as haloperidol (at a lower dose of 0.05mg/kg) are potentially promising adjunct modalities based on the level of evidence that we have to date.
References:
- Bollom A et al. Emergency Department Burden of Nausea and Vomiting Associated With Cannabis Use Disorder: US Trends From 2006 to 2013. J Clin Gastroenterol. 2018. PMID: 29095419
- Kim H et al. Cyclic vomiting presentations following marijuana liberalization in Colorado. Acad Emerg Med. 2015. PMID: 25903855
- Patel R et al. Burden of Persistent Vomiting With Cannabis Use Disorder: Report From 55,549 Hospitalizations in the United States. Psychosomatics. 2019. PMID: 31405569
- Allen J et al. Cannabinoid hyperemesis: cyclical hyperemesis in association with chronic cannabis abuse. Gut. 2004. PMID: 15479672
- Ruberto KH et al. Intravenous Haloperidol Versus Ondansetron for Cannabis Hyperemesis Syndrome (HaVOC): A Randomized, Controlled Trial. Ann Emerg Med. 2020. PMID: 33160719
- Witsil J et al. Haloperidol, a Novel Treatment for Cannabinoid Hyperemesis Syndrome. Am J Ther. 2017. PMID: 25393073.
- Narváez C et al. Cannabinoid hyperemesis syndrome. A report of six new cases and a summary of previous reports. Adicciones. 2016. PMID: 26990261
- de Moore GM et al. Psychogenic vomiting complicated by marijuana abuse and spontaneous pneumomediastinum. Aust N Z J Psychiatry. 1996. PMID: 8811275.
- Bonnet U et al. Cannabis-Hyperemesis-Syndrom [Cannabis hyperemesis syndrome]. Fortschr Neurol Psychiatr. 2012. PMID: 21692016.
- Hickey JL et al. Haloperidol for treatment of cannabinoid hyperemesis syndrome. Am J Emerg Med. 2013. PMID: 23583118.
- Jones J et al. Successful Treatment of Suspected Cannabinoid Hyperemesis Syndrome Using Haloperidol in the Outpatient Setting. Case Rep Psychiatry. 2016. PMID: 27597918
- Srihari P et al. Cannabinoid Hyperemesis Syndrome Associated With Compulsive Showering and Acute Kidney Injury. Prim Care Companion CNS Disord. 2016. PMID: 27247840
- Inayat F et al. Is haloperidol the wonder drug for cannabinoid hyperemesis syndrome? BMJ Case Rep. 2017. PMID: 28052951.
For More Thoughts on This Topic Checkout:
Post Peer Reviewed By: Salim R. Rezaie, MD (Twitter: @srrezaie)
The post The HaVOC Trial: IV Haloperidol vs Ondansetron for Cannabis Hyperemesis Syndrome appeared first on REBEL EM - Emergency Medicine Blog.
