
 Background: Perichondritis is an infection of the connective tissue of the ear that covers the cartilaginous auricle or pinna, excluding the lobule (Caruso 2014). The term perichondritis is itself a misnomer, as the cartilage is almost always involved, with abscess formation and cavitation (Prasad 2007). Perichondritis can be a devastating disease, and if left improperly treated, the infection can worsen into a liquefying chondritis resulting in disfigurement and/or loss of the external ear (Noel 1989) (Martin 1976). Unfortunately, misdiagnosis and mistreatment is common. In one small retrospective review, the overwhelming majority of patients presenting to a large general hospital were prescribed antibiotics without appropriate antimicrobial coverage, resulting in a significant number of patients developing chondral deformities or “cauliflower ear” (Liu 2013).
Background: Perichondritis is an infection of the connective tissue of the ear that covers the cartilaginous auricle or pinna, excluding the lobule (Caruso 2014). The term perichondritis is itself a misnomer, as the cartilage is almost always involved, with abscess formation and cavitation (Prasad 2007). Perichondritis can be a devastating disease, and if left improperly treated, the infection can worsen into a liquefying chondritis resulting in disfigurement and/or loss of the external ear (Noel 1989) (Martin 1976). Unfortunately, misdiagnosis and mistreatment is common. In one small retrospective review, the overwhelming majority of patients presenting to a large general hospital were prescribed antibiotics without appropriate antimicrobial coverage, resulting in a significant number of patients developing chondral deformities or “cauliflower ear” (Liu 2013).
Causes: A number of causes of perichondritis have been identified, with one study of 85 patients suggesting the most common causes including minor trauma, burns, and ear piercing (Prasad 2005). Notably, damage to the cartilage is not a necessary prerequisite—infection can occur if the overlying meatal skin is subjected to even trivial trauma, such as a scratch with an infected fingernail. In a significant percentage of cases, no significant cause can be identified (Prasad 2007) (Levin 1995). Nonetheless, several authors postulate that a growing incidence of perichondritis may be associated with the rising popularity of high chondral ear piercing, which causes stripping of the perichondrium and microfracture of the avascular cartilage while directly introducing infection (Prasad 2007) (Liu 2013). Perichondritis has been noted to be the presenting symptom of a number of disease processes marked by immunosuppression, including HIV-associated Non-Hodkin’s Lymphoma, relapsing polychondritis, and—not uncommonly—diabetes (Caruso 2014) (Levin 1995).
The most common microorganism responsible for perichondritis is Pseudomonas Aeruginosa, a gram-negative rod with intrinsic antibiotic resistance mechanisms (Caruso 2014) (Wu 2011). In one retrospective analysis of 61 patients with perichondritis, Pseudomonas was identified in 95% of cases. Co-infection with E. Coli was identified in half of cases, and Staph Aureus in 7% of patients. Because of the varying antibiotic sensitivities of these causative organisms, culture swab is recommended in all cases (Prasad 2005).
Diagnosis and Management: The diagnosis of perichondritis is clinical via physical exam. Patients initially experience dull pain, which gradually develops into severe otalgia with a purulent discharge (Noel 1989). Early cases are marked by erythema, swelling, and tenderness of the auricle without notable fluctuance (Chun 2013). The lobule remains unaffected, helping to distinguish perichondritis from otitis externa (Kullar 2012). A nidus of infection may be able to be identified within the superior fossae, though often will be absent. Complete clinical examination should exclude tenderness or fluctuance of the mastoid process of the temporal bone, as well as facial, orbital, or middle ear involvement.
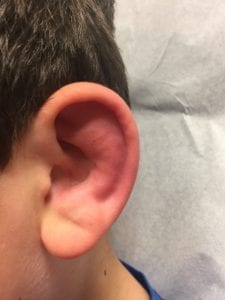
Management of perichondritis includes antibiotic therapy with anti-pseudomonal activity and consideration of incision and drainage by ENT specialists in the case of fluctuance in order to remove necrotic cartilage (Caruso 2014). Generally, appropriate outpatient antibiotic coverage would dictate oral therapy with ciprofloxacin or another fluoroquinolone, however the overall susceptibility of Pseudomonas has decreased steadily from 86% in 1994 to 76% in 2000, a result that has been significantly correlated to the increased use of fluoroquinolones (Wu 2011). Local antibiograms demonstrating antibiotic susceptibilities should guide empiric therapy, however. As high rates of oral antibiotic treatment failure have been documented, some patients may require a course of intravenous antibiotics or treatment in a monitored setting in order to ensure symptom improvement (Rees 2016). Indeed, as any lesion involving the pinna can have drastic and alarming cosmetic complications, some authors routinely recommend hospital admission for urgent specialist evaluation and parenteral therapy, particularly among pediatric patients (Prasad 2005).
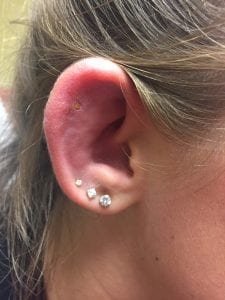
Traditionally, fluoroquinolones have been avoided in pediatric patients due to fears of arthropathy, however recent literature suggests that risk is abundantly low. In one meta-analysis of 16,184 pediatric patients given systemic ciprofloxacin, the risk of musculoskeletal adverse events attributed to therapy was 1.6%, half of which were arthralgias which resolved upon drug withdrawal (Adefurin 2011). In another comprehensive review of the literature from 1980 to 2007, four large retrospective studies failed to identify a significant link between musculoskeletal injury and fluoroquinolone treatment (Forsythe 2007). Ultimately, there are no studies demonstrating significant growth disturbance due to ciprofloxacin use, suggesting that a short course in reasonable and safe in pediatric populations in the context of appropriate monitoring and follow-up (Liu 2013).
Take-Home Points:
- Perichondritis is a pseudomonal infection of the outer ear marked by tenderness and erythema and distinguished by a spared lobule.
- Misdiagnosis or mistreatment can result in devastating patient outcomes.
- Treatment of perichondritis includes a foundation of anti-pseudomonal antibiotic therapy with or without surgical intervention.
- Urgent specialist evaluation and hospital admission should be considered when abscess or necrosis are suspected or patient follow-up may be challenging.
- Fluoroquinolone therapy appears safe in pediatric populations in the context of appropriate monitoring and follow-up.
References:
- Caruso, Andria M., Macario Camacho Jr, and Scott Brietzke. “Recurrent auricular perichondritis in a child as the initial manifestation of insulin-dependent diabetes mellitus: A case report.” ENT: Ear, Nose & Throat Journal 93.2 (2014). (PMID: 24526489)
- Prasad, H. Kishore C., et al. “Perichondritis of the auricle and its management.” The Journal of Laryngology & Otology 121.6 (2007): 530-534. (PMID: 17319983)
- Noel, Stella Boustany, et al. “Treatment of Pseudomonas aeruginosa auricular perichondritis with oral ciprofloxacin.” The Journal of dermatologic surgery and oncology. 15.6 (1989): 633-637. (PMID: 2723226)
- Martin, A.J. Yonkers, C.T. Yarington. Perichondritis of the ear Laryngoscope, 86 (1976), pp. 664-673 (PMID: 933656)
- Liu, Z. W., and P. Chokkalingam. “Piercing associated perichondritis of the pinna: are we treating it correctly?.” The Journal of Laryngology & Otology 127.5 (2013): 505-508. (PMID 23442437)
- Levin, Roger J., David H. Henick, and Alan F. Cohen. “Human immunodeficiency virus-associated non-Hodgkin’s lymphoma presenting as an auricular perichondritis.” Otolaryngology–Head and Neck Surgery 112.3 (1995): 493-495. (PMID: 7870459)
- Wu, Douglas C., et al. “Pseudomonas skin infection.” American journal of clinical dermatology 12.3 (2011): 157-169. (PMID: 21469761)
- Prasad KC, Karthik S, Prasad SC. A comprehensive study on lesions
- of the pinna. Am J Otolaryngol 2005;26(1):1-6. (PMID: 15635573)
- Chun, Robert, and Opeyemi Daramola. “Clinical Anatomy for the Pediatrician.” Otolaryngology for the Pediatrician 1 (2013): 3.
- Kullar, Peter, and Philip D. Yates. “Infections and foreign bodies in ENT.” Surgery (Oxford) 30.11 (2012): 590-596. (PMID: 27057069)
- Rees, Chris A., Daniel M. Rubalcava, and Corrie E. Chumpitazi. “A child with a painful swollen ear.” Archives of disease in childhood 101.9 (2016): 859. (PMID: 27102760)
- Adefurin A, Sammons H, Jacqz-Aigrain E, Choonara I. Ciprofloxacin safety in paediatrics: a systematic review. Arch Dis Child 2011;96:874–80 (PMID: 27185119)
- Forsythe, Clinton T., and Michael E. Ernst. “Do fluoroquinolones commonly cause arthropathy in children?.” Canadian journal of emergency medicine 9.6 (2007): 459-462. (PMID: 18072993)
Post Peer Reviewed By: Salim Rezaie (Twitter: @srrezaie)
The post Perichondritis: Not Just Simple Cellulitis appeared first on REBEL EM - Emergency Medicine Blog.
