
 Background: Fingertip amputations are not an uncommon injury seen in the emergency department. Treatment options range from healing by secondary intention to flap coverage or replantation. Selection of the appropriate treatment modality depends on the nature of the injury, the physical demands of the patient, and the patient’s co-morbidities. Prophylactic antibiotic use in patients with fingertip amputations is controversial. The routine use of prophylactic antibiotics is universally recommended on grossly contaminated wounds, in immunocompromised patients, and in injuries with extensively destroyed/devitalized tissue as it is thought the infection risk is high in these circumstances. However, many reflexively prescribe antibiotics prophylactically in all distal tip amputations. Moreover, there is often an underlying tuft fracture and we reflexively give these patients antibiotics because we were all taught that any open fractures require antibiotics in addition to usual fracture care. Prior studies on distal fingertip amputations and the use of prophylactic antibiotics suggest no change in infection risk with the routine use of antibiotics but these studies were small and have done little to inspire an antibiotic-restrictive approach universally.
Background: Fingertip amputations are not an uncommon injury seen in the emergency department. Treatment options range from healing by secondary intention to flap coverage or replantation. Selection of the appropriate treatment modality depends on the nature of the injury, the physical demands of the patient, and the patient’s co-morbidities. Prophylactic antibiotic use in patients with fingertip amputations is controversial. The routine use of prophylactic antibiotics is universally recommended on grossly contaminated wounds, in immunocompromised patients, and in injuries with extensively destroyed/devitalized tissue as it is thought the infection risk is high in these circumstances. However, many reflexively prescribe antibiotics prophylactically in all distal tip amputations. Moreover, there is often an underlying tuft fracture and we reflexively give these patients antibiotics because we were all taught that any open fractures require antibiotics in addition to usual fracture care. Prior studies on distal fingertip amputations and the use of prophylactic antibiotics suggest no change in infection risk with the routine use of antibiotics but these studies were small and have done little to inspire an antibiotic-restrictive approach universally.
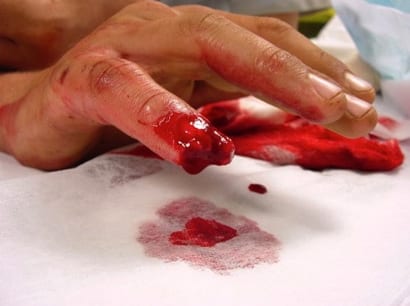
Clinical Question: Do antibiotics given prophylactically after debridement and repair of distal fingertip amputations lessen the risk of infection?
Article:
Rubin, G et al. The use of prophylactic antibiotics in treatment of fingertip amputation: a randomized prospective trial. Am J Emerg Med. 2015 May;33(5):645-7. PMID: 25682579
Population: All adults (≥ 18 yo) presenting to the Emergency Department at an Israeli hospital between May 2010 and May 2014 with a fingertip amputation with bone exposed.
Intervention: Admission to hospital for operating room (OR) wound management and parenteral prophylactic antibiotics (cefazolin, 1 g, 3 times daily) for 3 days.
Control: Admission to hospital for OR wound management without prophylactic antibiotics
Outcome: Infection (using clinical parameters of erythema, pain, swelling, wound discharge, or presence of purulence or cellulitis) at follow-up visits scheduled at 10 and 30 days
Design: Single center, prospective, randomized controlled trail
Excluded: <18 yo, patients with diabetes, an oncological disorder, an immune deficiency, or a bleeding disorder; patients who used steroids regularly; patients who presented with a grossly contaminated wound or other injury requiring antibiotic treatment; patients currently taking antibiotics; patients with a previous allergic reaction to cephalosporins
Primary Results
- 63 patients enrolled (but 6 excluded)
- 58 patients randomized with 60 finger injuries
- 27 patients allocated to antibiotic group and 31 patients allocated to no-antibiotic group
- No difference between groups in terms of sex, age, involved digit, mechanism of injury, time to OR, and type of surgery
Critical Findings
- NO infectious complications in either group
Strengths:
- Randomized controlled trial
- Study asked a clear clinical question with a patient centered outcome
- Exclusion criteria were reflective of current practice (we generally give most those patients excluded in this study antibiotics due to high risk for infection)
- Follow-up seemed complete (although little mention of this in publication)
Limitations:
- Small sample size
- Non-blinded
- Non-generalizable: management not consistent with current practice in most U.S. ED’s (these patient’s just don’t get admitted for OR washout and repair; most prophylactic antibiotics given in U.S. as outpatients and PO)
Other Issues:
- The numbers of patients don’t add up (63 recruited – 6 excluded = 57, not 58 total patients)
Authors’ Conclusions: “This study is the first to address the need for prophylactic antibiotic in adult fingertip amputation with bone exposed. In this study, we found no infection; and we attribute this result to the rarity of infection in this kind of injury, the small sample size, and the fact that all wounds were treated by debridement, irrigation, and rapid primary repair in and operating room environment. This study reinforce(s) the common belief that early meticulous wound care appears to be the most important factor in preventing infection in adult, healthy patients without grossly contaminated fingertip amputation.”
Our Conclusions: This study demonstrates that early and meticulous wound care is the key factor in preventing infection in healthy adults but is limited in its’ applicability to our practice setting so it does little to dispel the likely myth that prophylactic antibiotics prevent infection in fingertip amputations in healthy adults.
Potential to Impact Current Practice: It is difficult to recommend against the use of prophylactic antibiotics in our current practice setting for distal fingertip amputations managed in the ED based solely on this paper.
Bottom Line: Meticulous wound care early after injury limits risk of infection above all else. Prophylactic antibiotics may have no effect on infection risk for healthy adult patients with distal fingertip amputations. However, the data on these operating room managed patients cannot be extrapolated to patients debrided in the ED.
Guest Post By:
 Dan Silva, MD
Dan Silva, MD
PGY4 Resident
NYU/Bellevue EM Residency Program
Post Peer Reviewed By: Salim Rezaie (Twitter: @srrezaie)
The post Should We Give Fingertip Amputations with Exposed Bone Prophylactic Antibiotics? appeared first on REBEL EM - Emergency Medicine Blog.
